 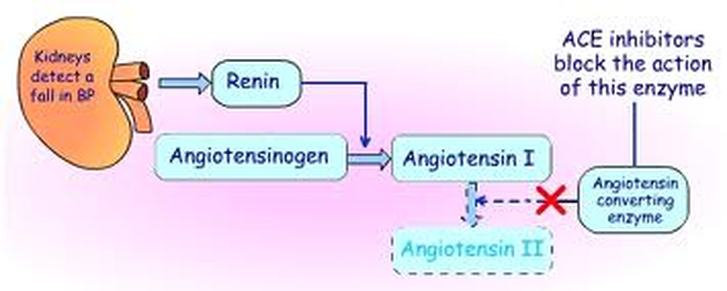
Thus, low-dose combination therapy (of a dihydropyridine calcium antagonist with either an ACE inhibitor or an ARB) may be preferred over high-dose monotherapy. In contrast, the addition of a diuretic has little effect on vasodilatory edema. The addition of an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin receptor blocker (ARB) to a dihydropyridine calcium antagonist significantly reduces vasodilatory edema. At an equal antihypertensive efficacy, lercanidipine and lacidipine are associated with less vasodilatory edema than amlodipine and nifedipine. 
Not all dihydropyridine calcium antagonists are created equal with regard to vasodilatory edema. Vasodilatory edema is dose-dependent and most common with direct arteriolar dilators such as minoxidil or hydralazine, and in decreasing order of frequency with the dihydropyridine calcium antagonists, a-blockers, antiadrenergic drugs, and nondihydropyridine calcium antagonists. Angiotensin-converting-enzyme (ACE) inhibitors are among the most widely used drugs in cardiovascular medicine, being effective antihypertensive agents, the vasodilator of choice in congestive heart failure, and a useful therapy in diabetic nephropathy. Serious side-effects that have been associated with enalapril include frequent or non-existent urination, fainting, fever, chills, bleeding, rapid weight gain. Vasodilatory edema, a common adverse effect of antihypertensive therapy with vasodilators, is related to several mechanisms, including arteriolar dilatation (causing an increase in intracapillary pressure), stimulation of the renin-angiotensin-aldosterone system, and fluid volume retention. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
